Knee Pain Without Surgery: 5 Treatments | R3BOOT

Dr. Hiral Parikh
8 May 2026
Knee Pain Treatment Without Surgery: 5 Options That Actually Work
Persistent knee pain does not automatically mean surgery. That is the first thing I tell clients who come to R3BOOT in Dadar, Mumbai, convinced that an operation is their only way out.
In most cases, it isn't.
Clinical guidelines consistently recommend structured conservative care before surgical referral. Research shows that for conditions like osteoarthritis and patellofemoral pain, targeted physiotherapy and load management produce outcomes comparable to surgery in many patients, without the recovery time or the risk.
But the key word is "structured." Knee pain treatment without surgery only works when the right options are applied in the right order, matched to the right diagnosis.
Here is what that looks like in practice.
What Kind of Knee Pain Responds to Non-Surgical Treatment?
Most persistent knee pain responds well to conservative care. The conditions that benefit most include osteoarthritis, patellofemoral pain syndrome (pain around or behind the kneecap), meniscal irritation without locking, IT band syndrome, and general overuse or training-related joint pain.
The conditions where surgery is more likely to be needed include mechanical locking caused by a torn meniscus fragment, complete ligament ruptures requiring reconstruction, and severe structural deformity with significant joint space loss.
A proper clinical diagnosis is the starting point. Not a guess based on where it hurts. At R3BOOT, every new knee client begins with a movement screen and a structured assessment before any treatment plan is recommended. If imaging is needed, we review it together with your activity goals so the plan reflects both the scan and the person.
If your diagnosis is unclear, clarify it before spending money on treatment. The wrong treatment for the wrong diagnosis is not conservative care. It is wasted time.
Option 1: Physiotherapy for Knee Pain (The Non-Negotiable Starting Point)

What does physiotherapy actually do for knee pain?
Targeted physiotherapy reduces knee pain by improving the strength, control, and loading capacity of the muscles and tissues around the joint. It does not regrow cartilage, but it does change how much load the joint absorbs, how efficiently it moves, and how well the surrounding structures protect it under stress.
This matters because most persistent knee pain is a load management problem, not an irreversible structural one.
Systematic reviews consistently show that supervised exercise therapy reduces pain and improves function in knee osteoarthritis. Research published in the British Journal of Sports Medicine reports that exercise is as effective as surgery for many people with meniscal tears. For patellofemoral pain, structured quadriceps and hip strengthening produces reliable, durable improvements.
Dr. Hiral Parikh holds a Bachelor's degree in Physiotherapy from Maharashtra University of Health Sciences. At R3BOOT, she works with athletes and active adults across rehabilitation, pain management, and movement therapy, building recovery plans around each patient's specific deficits and goals.
In our clinic, when clients come to us with persistent knee pain that has not responded to rest or generic exercises, the problem is almost always specificity. The exercises they have been doing are either too easy, too random, or not matched to what their knee actually needs.
What a proper physiotherapy programme looks like
A structured programme at R3BOOT's physiotherapy clinic in Dadar moves through five phases:
Baseline assessment and movement screen to identify load faults, strength deficits, and movement compensations.
Foundation strength work targeting quadriceps, hamstrings, hip abductors, and calf, at loads the joint can currently tolerate.
Neuromuscular control training to retrain how the knee tracks and absorbs force during real movement.
Progressive load reintroduction with monitored progression criteria so you're not guessing when to move forward.
Sport- or activity-specific conditioning so you return to what you do, not just a generic functional baseline.
Clinical trial protocols typically run twice-weekly supervised sessions for 8 to 12 weeks, combined with structured home practice. Most clients report meaningful pain reduction within 6 weeks when the programme is targeted correctly.
Call R3BOOT on +91 9702368612 to book your diagnostic movement screen if you've been managing knee pain on your own for more than 4 weeks without clear improvement.
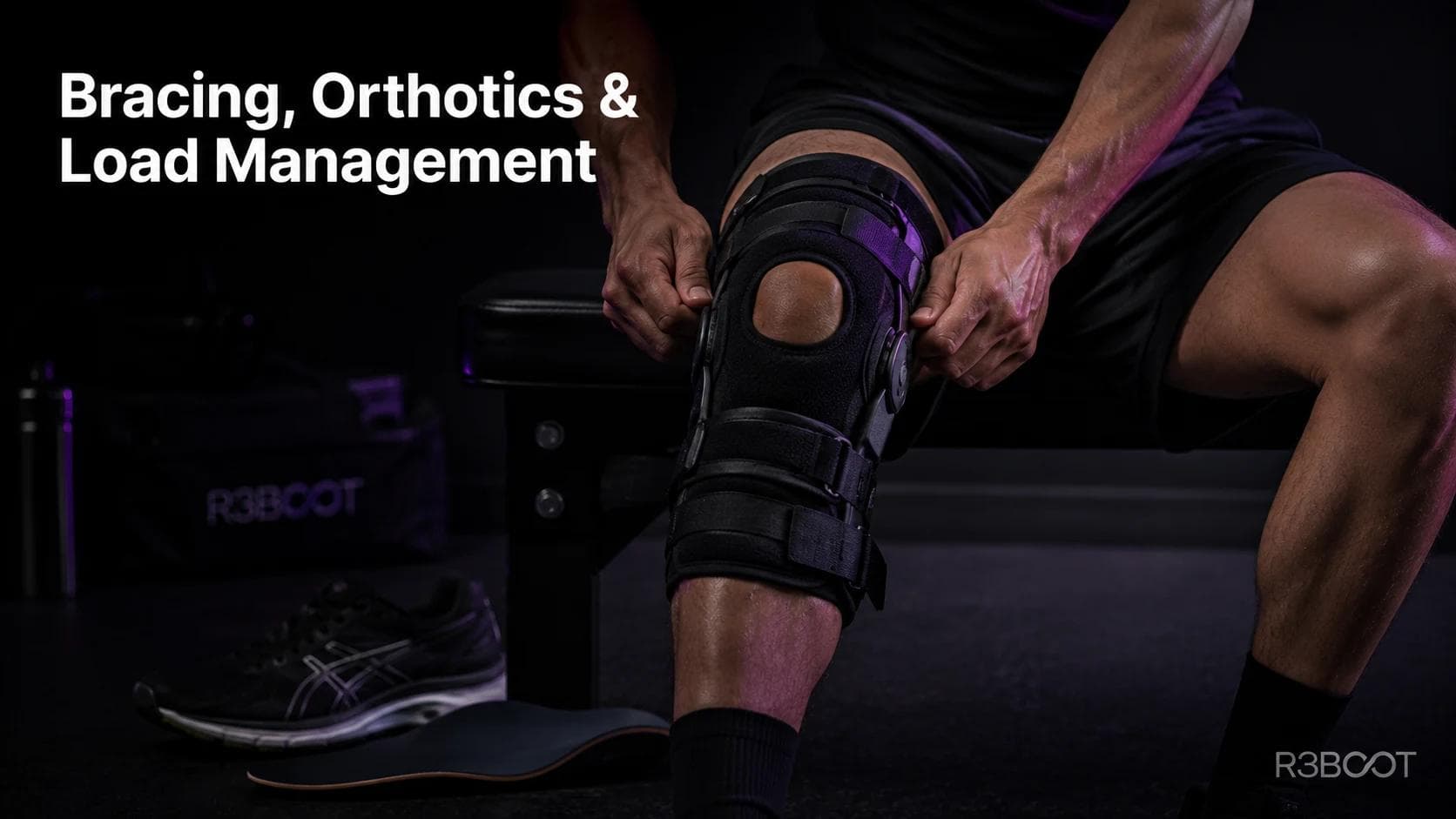
Option 2: Bracing, Orthotics, and Load Management
Can a brace or insole actually reduce knee pain?
Yes, but not by fixing the problem. Bracing and orthotics work by altering joint mechanics: changing the direction of load through the knee, reducing compressive force on a specific compartment, or providing external stability cues when the surrounding muscles can't yet provide them.
The benefit is fast. The risk is dependency if not paired with strengthening.
Knee unloader braces are supported by evidence for medial compartment osteoarthritis, shifting load away from the damaged side and reducing pain enough to participate in rehabilitation. Patellofemoral bracing and taping help with kneecap tracking pain, particularly in the short term. Custom orthotics are most useful when foot mechanics (overpronation, for example) are contributing to knee load patterns.
The correct approach is to use a brace or orthotic as a tool to create a pain window, then fill that window with the strengthening work that makes the support progressively less necessary.
Load management, meaning the deliberate reduction and controlled reintroduction of training volume, is also underused. Persistent knee pain often comes from doing too much too fast after a period of inactivity, or from cumulative training load that the joint hasn't adapted to. A structured load reduction of 20 to 30% over 2 weeks, combined with physiotherapy, often produces more improvement than months of pain management alone.
Option 3: Medications for Knee Pain (What Helps, What Doesn't)

Medications in non-surgical knee pain management serve one purpose: symptom control that enables participation in rehabilitation. They are not a long-term solution on their own.
Topical NSAIDs (like diclofenac gel) are the first-line recommendation from NICE guidelines for osteoarthritis. They reduce local inflammation with fewer systemic side effects than oral options and work well for accessible joints like the knee.
Oral NSAIDs (ibuprofen, naproxen) are appropriate for short-term flare management. They are not appropriate for long-term daily use due to gastrointestinal and cardiovascular risk, particularly in older clients.
Paracetamol provides modest short-term relief in some patients. Evidence for its benefit in knee osteoarthritis is weaker than commonly assumed; use it if topical options are insufficient, not as the primary strategy.
Avoid over-relying on painkillers to push through training loads that your knee currently cannot handle. That is not recovery. That is suppressing feedback that your body is trying to give you.
Option 4: Injections for Knee Pain (Corticosteroid, Hyaluronic Acid, PRP)
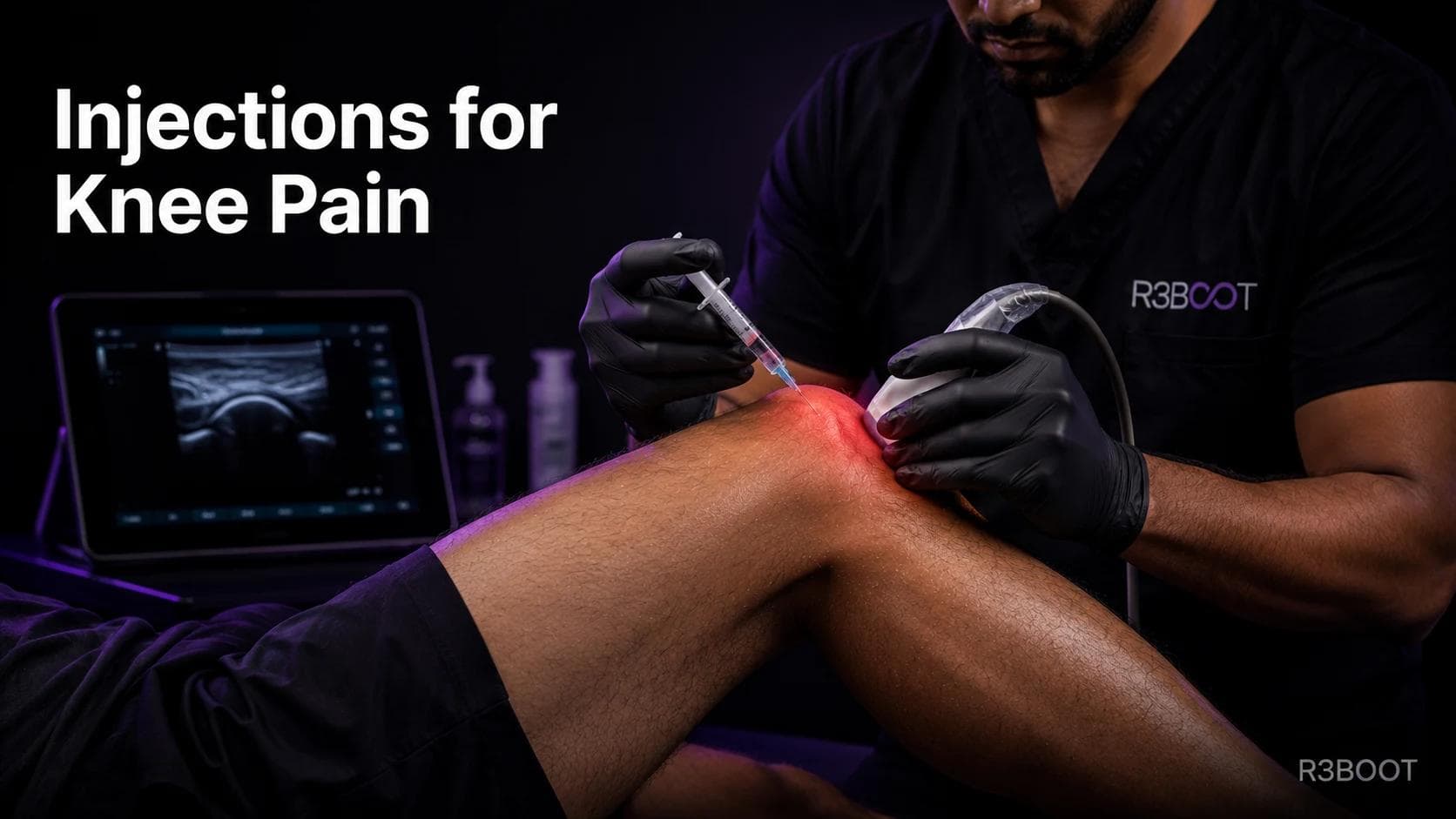
When are knee injections the right choice?
Injections become relevant when supervised physiotherapy has reduced pain but not eliminated it, or when a severe acute flare prevents participation in rehabilitation altogether. They are a selective tool, not a first step.
Corticosteroid injections provide reliable short-term pain relief, typically lasting 4 to 12 weeks. They work by reducing intra-articular inflammation rapidly. They are best used to control a severe flare so that rehabilitation can continue. Repeated use increases the risk of tissue weakening and, in some cases, accelerated cartilage changes, so frequency matters. Most clinicians recommend no more than two to three injections per joint per year.
Hyaluronic acid (visco-supplementation) injections aim to restore the lubricating properties of joint fluid. Evidence is mixed. A Cochrane review found modest short-term benefit compared to placebo for some patients with mild to moderate osteoarthritis. They are more appropriate for clients who want medium-term relief and cannot tolerate NSAIDs.
Platelet-Rich Plasma (PRP) uses a concentration of your own blood's growth factors to promote tissue healing. Evidence is emerging but still inconsistent. Some studies show superior pain reduction compared to corticosteroids at the 6-month mark, particularly in younger patients with early osteoarthritis or soft tissue pathology. It is not a standard first-line option but is reasonable for clients who have not responded to corticosteroid or hyaluronic acid.
All injections should be used alongside rehabilitation. An injection without a structured physiotherapy plan is a temporary fix that solves nothing.
Option 5: Minimally Invasive Procedures and When to Consider Surgery
What options exist between injections and joint replacement?
When injections and physiotherapy have both been genuinely tried over 10 to 12 weeks and pain remains functionally limiting, a specific minimally invasive option exists before joint replacement is considered.
Genicular nerve radiofrequency ablation (RFA) targets the small nerves that carry pain signals from the knee joint. A diagnostic nerve block is performed first: if it reduces pain significantly, RFA is likely to work. When successful, it provides 6 to 12 months of pain relief, sometimes longer, and enables continued rehabilitation without pain as the limiting factor.
RFA does not repair the joint. It reduces the pain signal. It is appropriate for patients with focal, well-localised knee pain who are not yet candidates for or do not want joint replacement surgery.
When does surgery become the right answer?
Surgery becomes appropriate when structured, measured conservative care has failed over at least 12 weeks, or when specific red flags are present.
Red flags that indicate surgical review should not be delayed:
- Mechanical locking or catching (the knee actually gets stuck mid-movement)
- Progressive angular deformity (the leg is visibly bowing or collapsing)
- Large recurrent effusions (the knee keeps filling with fluid)
- Severe instability that prevents normal walking
- Continuous night pain that does not respond to any conservative treatment
- Imaging showing Kellgren-Lawrence grade 3 to 4 changes with symptoms that match
If any of these are present, request a surgical opinion. The goal is not to avoid surgery at all costs. The goal is to reach surgery only when it is genuinely necessary, so that when it happens, you're going in strong and recovering effectively.
A Practical 8-to-12 Week Non-Surgical Plan for Knee Pain
If you want a structured starting point, this is how a rational escalation looks:
Weeks 1 to 4: Begin supervised physiotherapy. Get a proper diagnosis. Add a brace or orthotic if mechanical malalignment is a factor. Reduce load by 20 to 30% from your current activity levels.
Weeks 2 to 6: Use topical NSAIDs for symptom management. Consider a corticosteroid injection if pain prevents participation in physiotherapy.
Weeks 4 to 8: Progress physiotherapy loads. Reassess pain and function against your baseline. If progress is inadequate, consider hyaluronic acid or PRP.
Weeks 8 to 12: If pain remains functionally limiting despite full engagement with the above, explore genicular nerve block as a diagnostic and therapeutic step. If red flags are present at any stage, escalate to surgical review immediately.
Set measurable goals before you start. "Less pain" is not a measurable goal. "Return to 5km running without pain by week 10" is. Goals give you a decision framework so you're not making emotional, reactive choices when progress is slow.
Our team at R3BOOT's integrated recovery centre in Dadar, Mumbai can help you map this entire pathway. If you're already part-way through and unsure where you stand, call us on +91 9702368612 to book a structured reassessment.
What Not to Do When Managing Knee Pain Without Surgery
This matters as much as the treatment list above.
Do not rest completely and wait. Deconditioning worsens most knee pain conditions. The joint needs graduated load to recover.
Do not use painkillers to train through increasing pain. Pain that worsens during or after exercise is a signal that load is exceeding capacity. Suppressing that signal with medication does not increase capacity. It hides the problem until it becomes a bigger one.
Do not rely on a brace indefinitely without addressing the underlying weakness. A brace that you need forever is a sign that the rehabilitation programme hasn't been completed.
Do not delay physiotherapy because injections are available. Injections control symptoms. Physiotherapy changes the underlying cause. Both have a role, but in the right order.
Sports massage is a useful adjunct for managing surrounding muscle tension during a physiotherapy programme but is not a standalone treatment for joint pain. Use it to support your rehab, not replace it.
Frequently Asked Questions
Can knee pain really be treated without surgery?
Yes, in most cases. Clinical guidelines recommend structured conservative care as the first-line treatment for persistent knee pain from conditions like osteoarthritis and patellofemoral pain. Research shows that supervised physiotherapy, load management, and appropriate injections restore meaningful function for the majority of patients. Surgery is reserved for defined failures of conservative care and specific structural problems that cannot be managed any other way.
How long does non-surgical knee pain treatment take?
Expect 8 to 12 weeks of structured treatment before you can assess whether conservative care is working. Pain reduction often begins within 3 to 6 weeks of starting a targeted physiotherapy programme. Full functional recovery, meaning return to sport or previous activity levels, typically takes 12 to 24 weeks depending on the diagnosis, severity, and consistency of the programme.
Is physiotherapy effective for knee osteoarthritis?
Yes. Multiple systematic reviews show that supervised exercise therapy reduces pain and improves function in knee osteoarthritis. The NICE guideline on osteoarthritis lists exercise as a core treatment. The key is that the programme must be targeted to the individual's specific deficits, not generic. A structured strength and neuromuscular programme outperforms unguided home exercise for most patients.
What is the difference between corticosteroid and PRP injections for knee pain?
Corticosteroid injections reduce inflammation quickly, providing reliable short-term relief (4 to 12 weeks) and are best used to manage flares so rehabilitation can continue. PRP injections use concentrated growth factors from your own blood to support tissue healing. Evidence suggests PRP may produce more durable benefits at 6 months compared to corticosteroids, particularly in younger patients or those with soft tissue pathology. Neither replaces physiotherapy.
When should I stop trying non-surgical treatment and consider surgery?
Seek a surgical opinion if: (1) structured conservative care including physiotherapy, load management, and at least one injection has failed over 12 weeks and function remains unacceptably limited; (2) you experience mechanical locking, severe instability, or continuous night pain; or (3) imaging shows significant joint space loss (Kellgren-Lawrence grade 3 to 4) with symptoms that match the structural findings. The decision should be based on objective failure criteria, not frustration with slow progress.